When any one is suffering from long illness like HIV, TB, cancer, or diabetes — and also malnutrition — the problem is not only in body but also in mind. Chronic (longterm) sickness makes people tired, worried, hopeless, and sometimes ashamed. When mind becomes weak, body also stop fighting.
For this reason, mental health support is as important as medicine or food in managing malnourished patients with chronic illness.
Understanding the Link Between Body and Mind
When a person is sick for long time, he lose weight, energy, and hope. Low nutrition affects brain chemicals that control mood, so malnourished patients often feel sad or anxious. On the other hand, depression reduces appetite — making nutrition even worse.
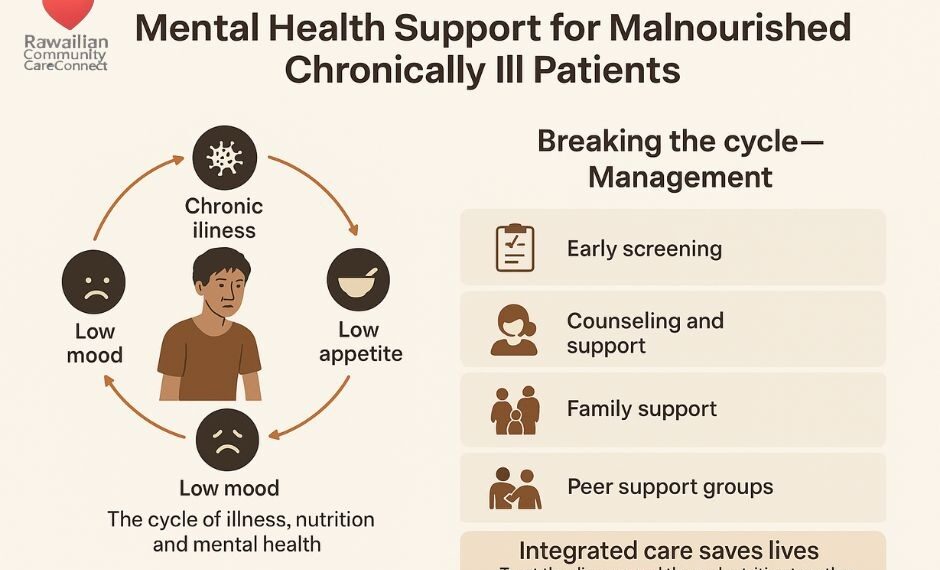
This creates a vicious cycle:
Illness → Poor appetite → Weak body → Low mood → Less eating → More weakness.
Breaking this cycle needs both nutrition and emotional support.
Common Mental Health Problems in Chronically Ill and Malnourished Patients
Depression: Feeling of sadness, no interest in life, low appetite, poor sleep.
Anxiety: Fear of disease, fear of death, worry about family or treatment cost.
Hopelessness and Low Self-Esteem: Thinking “I am useless” or “I will never recover.”
Stigma: Especially in HIV or TB, people hide their condition, which increase loneliness.
Irritability or Aggression: From stress, pain, or hunger.
These emotional problems affect how patient follow diet and treatment. A depressed patient will not eat even if food is available.
Why Mental Health Support is Important
Improves appetite and nutrition intake.
Helps medicine adherence — patient take drugs on time.
Reduces stress hormones that damage body.
Gives motivation to recover.
Strengthens relationship with family and caregivers.
How to Provide Mental Health Support
1. Early Screening
Health workers should check not only body signs but also emotional condition. Simple questions like “Do you feel sad most days?” or “Do you have trouble sleeping?” can help identify depression early.
2. Counseling and Listening
Give patient time to talk about fear and worry.
Listen without judgment or blame.
Offer hope — explain that with food, medicine, and care, life can improve.
Use simple language and respect local beliefs.
3. Family Support
Family is main emotional system in Pakistani culture. When family show love, patient feel stronger. Encourage family to sit, eat, and talk with patient daily. Teach them not to blame the sick person or show pity, but to show respect and encouragement.
4. Peer Support Groups
For HIV, TB, or dialysis patients, meeting other people with same condition reduce isolation. Peer groups share experience, coping tips, and give hope.
5. Nutrition and Mental Health Link
Some nutrients like iron, zinc, omega-3, and vitamin B help mood regulation. Balanced meals improve not only body but also brain function. Encourage patient to eat small frequent meals with natural colors — vegetables, fruit, eggs, and pulses.
6. Faith and Cultural Strength
Religious belief is strong source of comfort for many patients in Pakistan. Prayers, positive faith, and community support can bring peace and hope. However, patients should not replace medicine or diet with only faith healing — both are needed together.
7. Professional Help
If patient show serious depression (no eating, no sleep, talking about death), refer to psychologist or psychiatrist. In hospitals or clinics, short counseling sessions can be arranged.
Challenges in Pakistan
Limited number of mental health professionals.
Stigma toward mental illness.
Lack of integration of psychology with nutrition and medical care.
Families often focus only on physical recovery.
To improve this, hospitals and nutrition programs should train health staff in basic counseling and mental health first aid.
Practical Tips for Health Workers and Caregivers
Speak kindly and slowly; never blame the patient.
Encourage small daily goals — “Let’s try to eat one more spoon today.”
Celebrate small improvements (gaining weight, eating full meal, better sleep).
Maintain calm and friendly tone during visits.
Avoid forcing food; instead, create comfort and trust.
Conclusion
A healthy body cannot exist without a healthy mind. In chronic illness and malnutrition, both need care together. Mental health support — through listening, counseling, family love, and positive community attitude — helps patients recover faster and live with dignity.
“Nutrition feeds the body, but hope feeds the will to live.”
All doctor, nurse, and family member should remember: treating depression, anxiety, and loneliness is part of nutrition therapy. Healing must include both food for body and care for the mind.
Discover more from Rawallian Community CareConnect
Subscribe to get the latest posts sent to your email.