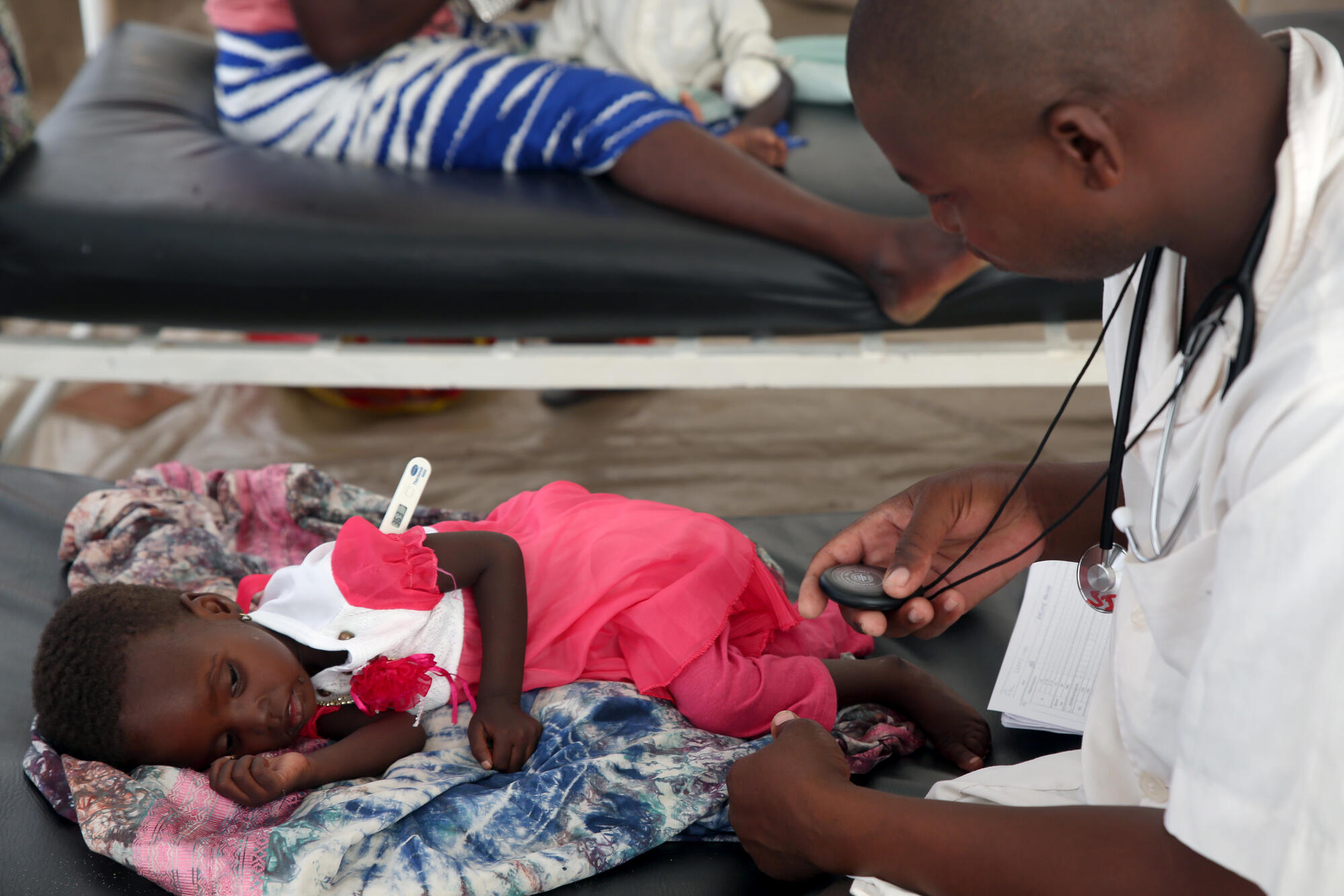
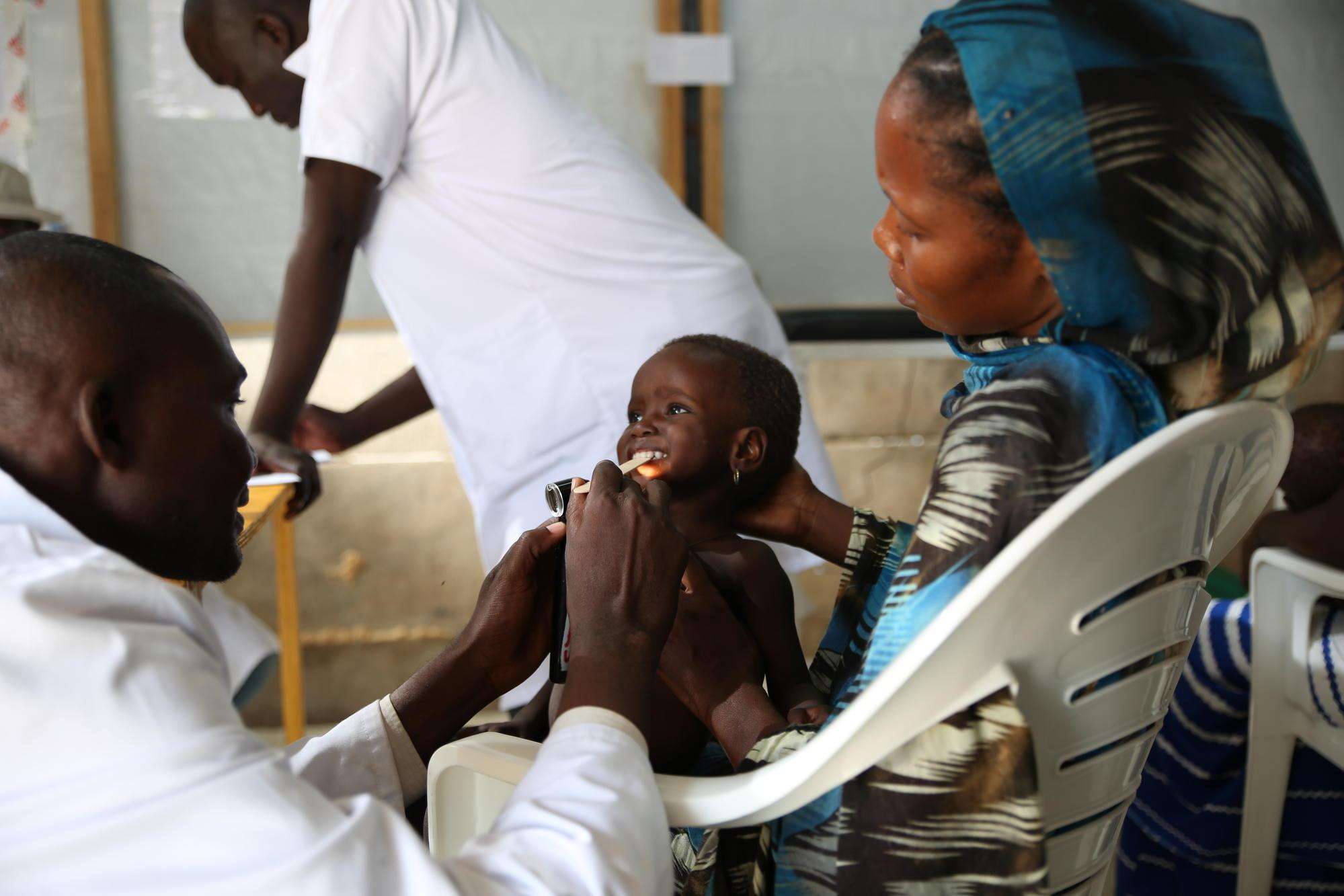
10 Tips on Psychological Care for a Severely Malnourished Child
Severe Acute Malnutrition (SAM) is a life-threatening condition where a child’s body lacks essential nutrients, often leading to extreme weight loss, swelling, and complications like infections or dehydration. It affects millions of children worldwide, especially in low-resource areas. Beyond physical health, SAM can harm a child’s mental and emotional development, causing delays in thinking, movement, and social skills, as well as anxiety or depression. Caregivers may also feel stressed or depressed. The good news is that combining nutritional treatment with psychological care—through play, emotional support, and stimulation—can help children recover better and develop normally. This article shares 10 simple tips for psychological care, based on guidelines from experts like the World Health Organization (WHO). Always work with healthcare professionals for personalized advice.
What Is SAM and Its Psychological Effects?
SAM happens when children don’t get enough food or absorb nutrients properly, often due to poverty, illness, or emergencies like conflicts. Children with SAM and complications need hospital care first to stabilize their health. Psychologically, malnutrition can lead to poor brain development, making kids less active, irritable, or withdrawn. They might show behaviors like rocking or not responding to others. Without support, these issues can last long-term, affecting learning and emotions. Psychological care helps by stimulating the senses, building bonds, and involving families, improving recovery rates and reducing risks like relapse or death.
10 Tips for Psychological Care
Here are 10 practical tips to support the mental and emotional well-being of a child with SAM and complications. These can be used in hospitals, at home, or in community programs.
- Involve Caregivers as Partners: Keep mothers or caregivers with the child during treatment. Encourage them to comfort, feed, bathe, and play with the child. This builds strong bonds and provides emotional security. Train caregivers on how to interact playfully to continue support at home.
- Create a Cheerful Environment: Decorate treatment areas with bright colors, pictures, and safe spaces. Avoid isolating the child—keep them in a stimulating, positive setting to prevent sensory deprivation and boost mood.
- Provide Daily Sensory Stimulation: Use activities that engage sight, sound, touch, and movement, like showing colorful objects, playing soft music, or gentle massages. For infants, focus on skin-to-skin contact to strengthen attachment. Aim for 15-30 minutes a day once the child is stable.
- Incorporate Structured Play Therapy: Organize short play sessions with simple toys like balls, blocks, or homemade items from bottles and cloth. Play helps develop motor skills, language, and social abilities. Make it family-centered by involving siblings or parents.
- Offer Tender Loving Care: Give the child lots of affection, hugs, and reassurance. Limit the number of adults interacting with them to avoid overwhelming, and ensure all contacts are warm and consistent. This reduces anxiety and helps with emotional recovery.
- Encourage Physical Activity Gradually: As the child improves, promote movement like crawling, walking, or simple exercises. This supports gross motor skills and overall development, combined with nutrition.
- Screen and Support Maternal Mental Health: Check caregivers for depression using simple tools like questionnaires. Offer counseling or group support, as a healthy caregiver can better care for the child. Address family stresses like poverty or trauma.
- Teach Parenting and Prevention Skills: Educate families on feeding, hygiene, and responsive caregiving. Use demonstrations to show how to respond to the child’s cues, preventing future malnutrition and building confidence.
- Monitor for Behavioral Issues: Watch for signs like irritability, withdrawal, or repetitive movements. Provide special attention and play to address them, and seek professional help if needed.
- Plan Follow-Up Care Post-Discharge: Continue stimulation at home with visits from health workers for 6-12 months. Provide toys and check progress to sustain gains and prevent relapse.
Discover more from Rawallian Community CareConnect
Subscribe to get the latest posts sent to your email.